Experts Say Risks Of A Common Allergy Medication May Weigh Out Its Benefits
For decades, millions of people have reached into their medicine cabinets for quick relief from sneezing, itching, and watery eyes. Yet a growing chorus of medical experts now warns that one of the most widely used allergy medications could pose more harm than help. In a new review, experts call for the removal of diphenhydramine from over-the-counter and prescription markets in the United States, saying it’s outdated, dangerous and eclipsed by safer alternatives. The medication, commonly known by its brand name Benadryl, has been a household staple since its approval in the mid-1940s, but recent research suggests its risks may be too significant to ignore. In a review published in February, allergy experts from Johns Hopkins University and the University of California, San Diego called for the removal of diphenhydramine from over-the-counter and prescription markets in the United States, saying it’s outdated, dangerous and eclipsed by safer alternatives.
The Hidden Dangers of a Common Medication
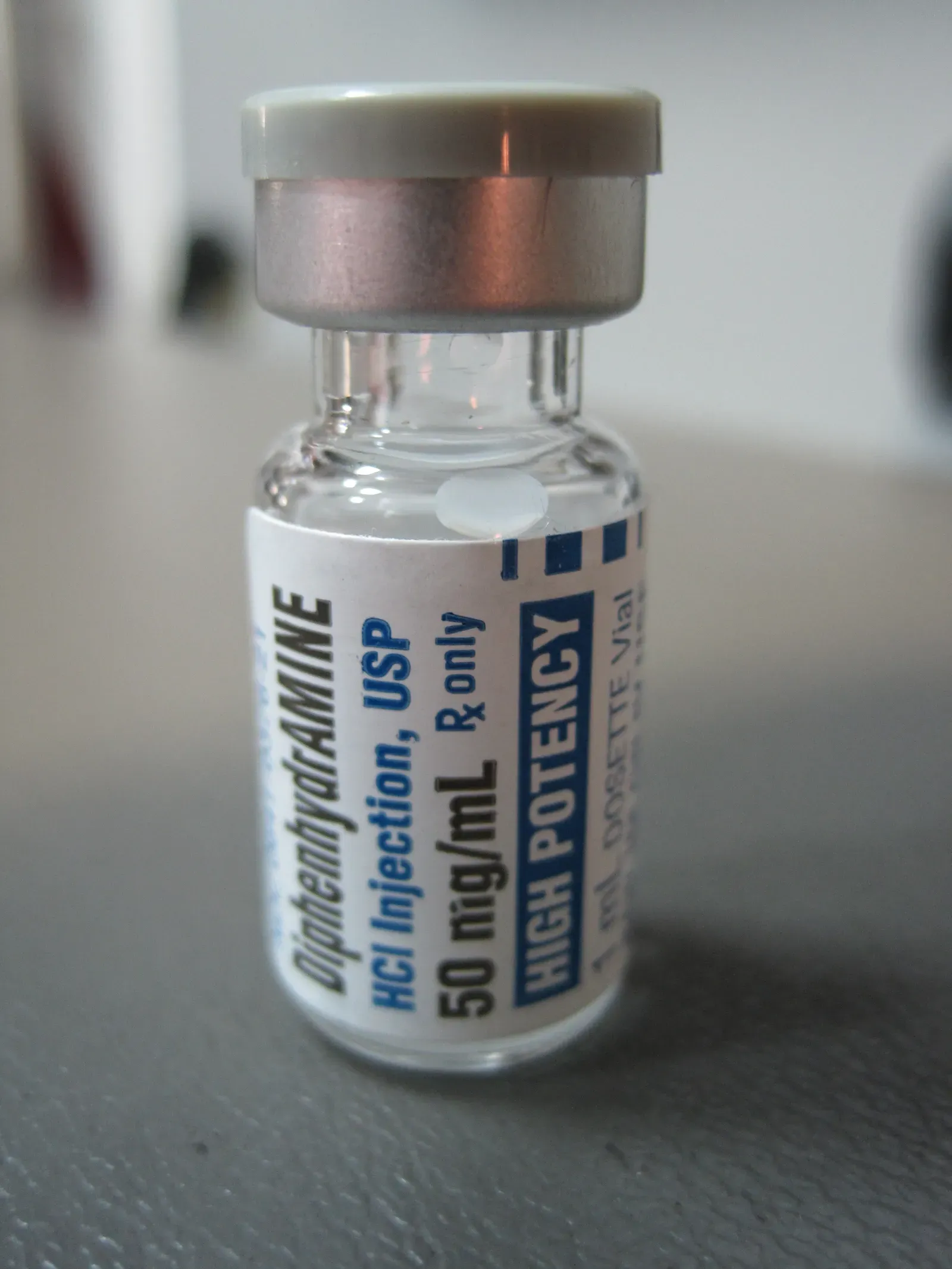
A first-generation antihistamine approved in 1946, diphenhydramine is widely used for allergies, sleep aid and cold symptoms. It’s a common over-the-counter medication in the US, with usage rising in the summer months as people use it to treat itching from bug bites or poison ivy, as well as sneezing and runny nose caused by grass and pollen allergies, according to the American Pharmacists Association. Still, medical professionals have raised concerns about the drug’s side effect profile. Diphenhydramine often causes sedation, cognitive impairment, and in some cases, dangerous cardiac effects, the authors wrote. In older adults, the drug can stay in the body for up to 18 hours, resulting in lingering sleepiness, disorientation and increasing risk of falling. These effects aren’t merely inconvenient – they can fundamentally disrupt daily life and safety.
The review also highlighted a possible link between long-term diphenhydramine use and dementia. This connection has become increasingly clear through multiple research studies conducted over the past decade. The increased risk of falls and cognitive decline in older adults has led to restrictions on the use of first-generation antihistamines, particularly diphenhydramine. QT prolongation and cardiotoxicity are concerns in at-risk populations. The medical community has become particularly worried about how these effects compound in vulnerable populations, especially those already at risk for memory problems or heart conditions.
The Dementia Connection That Changed Everything
Perhaps the most alarming finding about diphenhydramine centers on its potential connection to dementia and Alzheimer’s disease. Taking an anticholinergic for the equivalent of three years or more was associated with a 54% higher dementia risk than taking the same dose for three months or less. This finding comes from research tracking nearly three and a half thousand older adults over multiple years. The drug works by blocking acetylcholine, a brain chemical crucial for memory and learning functions.
Dr. Shelly Gray et. al. found a persistent link between dementia and some medications in a University of Washington/Group Health study published in JAMA Internal Medicine on January 26, 2015. The large study links a significantly increased risk for developing dementia, including Alzheimer’s disease, to taking commonly used medications with anticholinergic effects at higher doses or for a longer time. Researchers emphasized that the connection wasn’t limited to prescription medications. Many people taking over-the-counter sleep aids containing diphenhydramine remained unaware they were consuming the same active ingredient found in allergy medications, potentially doubling or tripling their exposure without realizing it.
Safer Alternatives Exist and Work Well

Medical professionals stress that effective alternatives to diphenhydramine are readily available and pose significantly fewer risks. Patients should trial alternatives agents like loratadine, which is Claritin, or cetirizine, which is Zyrtec, or fexofenadine, which is Allegra, to alleviate allergy symptoms, according to Dr. James Clark of the Department of Otolaryngology-Head and Neck Surgery at the Johns Hopkins University School of Medicine. These second-generation antihistamines work just as effectively for most people without crossing into the brain as readily as their older counterparts.
High-quality trials have proven that newer generation AHs are superior in safety compared to older first-generation AHs. On average, they have improved potency and efficacy. The Canadian Society of Allergy and Clinical Immunology has taken a strong position on this matter. The CSACI, therefore, recommends in agreement with other international bodies, that only less-sedating newer generation AHs should be first-line and preferred over older AHs and that the use of first-generation AHs should be significantly curtailed. First-generation AHs are associated with significant and, at times, serious adverse effects including fatal outcomes, and they should not be used as first-line treatment in allergic disease.
Recent FDA Warnings Add New Concerns

Even newer antihistamines have recently come under scrutiny for different reasons. The FDA is warning that patients stopping the oral allergy medicines cetirizine (Zyrtec) or levocetirizine (Xyzal) after long-term use may experience rare but severe itching. This warning, issued in May 2025, highlights yet another complexity in managing allergies with medication. The itching, also called pruritus, has been reported in patients who used these medicines daily, typically for at least a few months and often for years. Patients did not experience itching before starting the medicines. Reported cases were rare but sometimes serious, with patients experiencing widespread, severe itching that required medical intervention.
The FDA found 209 cases of itching after stopping these antihistamines worldwide. Tens of millions of people take these medicines daily. This means the number of reported cases are very few compared to how many people take these medicines, and the odds this issue may affect you would be very rare. Healthcare professionals now recommend that patients planning to discontinue these medications should consult with their doctors about gradually tapering doses rather than stopping abruptly. Despite this warning, medical experts emphasize that these second-generation medications remain far safer than first-generation options like diphenhydramine.
International Actions Reflect Growing Concerns

The United States isn’t alone in recognizing the problems associated with first-generation antihistamines. Countries outside the United States, including Germany, the Netherlands, and Sweden, have taken action to limit diphenhydramine’s accessibility by making it available by prescription only. Canadian, United States. and British healthcare agencies recommend against cold medications containing diphenhydramine for children younger than 5 (United States) and 6 (Canada and Britain). These international restrictions reflect a global recognition that the risks of these older medications may no longer justify their easy availability.
Despite its well-documented problematic therapeutic ratio, diphenhydramine remains available in over 300 formulations, most of which are over-the-counter. Based on a comprehensive evaluation of practice patterns and the prevalence and incidence of adverse clinical events, we believe that diphenhydramine has reached the end of its life cycle, and in its class of therapies it is a relatively greater public health hazard. We recommend it should no longer be widely prescribed or continue to be readily available over the counter. The availability of the drug in so many different products means many consumers may not even realize when they’re taking it, particularly when it appears in combination medications marketed for sleep, colds, or pain relief.
What Patients Should Do Now

Healthcare professionals recommend that anyone currently taking diphenhydramine regularly should speak with their doctor about switching to safer alternatives. Those who need allergy relief should consider second-generation antihistamines, which provide effective symptom control without the cognitive and cardiac risks. Second-generation antihistamines, such as those in Claritin and Zyrtec, along with steroid-based nasal sprays such as Flonase, will counteract allergy symptoms without targeting acetylcholine receptors, according to specialists in allergy and immunology.
People should also review all their medications, including over-the-counter products and sleep aids, to check whether they contain diphenhydramine or other anticholinergic ingredients. Many products use different brand names, making it easy to accidentally take multiple medications containing the same active ingredient. In the past, it has been a useful medication that has helped millions of patients; however, its current therapeutic ratio is matched or exceeded by second-generation antihistamines, especially due to their markedly reduced adverse reactions. It is time to say a final goodbye to diphenhydramine, a public health hazard, the authors wrote in their review.






